Professional insights:
Updated: December 30, 2025
RN and Other Nursing Careers to Pursue in 2025
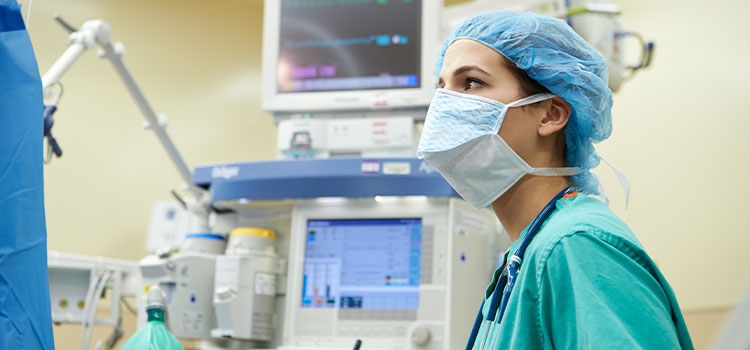
If you are compassionate and want to make a difference in people’s lives, 2025 is a great time to pursue a career in nursing. Nurses have long been recognized as some of the most trusted healthcare providers. Plus, the healthcare industry is growing rapidly and nurses are a big part of the expansion.
Among the benefits of nursing, nurses can often choose when and where to work, with the opportunity to choose from full-time, part-time, and per diem positions. Here’s a look at the careers you should consider pursuing in 2024.
Licensed Practical Nurse (LPN)
One of the fastest ways to become a nurse is by earning a licensed practical nurse (LPN) certification. LPNs work under the supervision of registered nurses (RNs) and other healthcare providers. They monitor vital signs, perform routine assessments and interventions, administer medications, and communicate with members of a patient’s care team.
LPNs “work as the eyes and ears of a healthcare provider or a registered nurse,” says Marla Kniewel, EdD, MSN, RN, the director of the MSN program and chair of the Institutional Review Board at Nebraska Methodist College. “They recognize that interprofessional collaboration among health care professionals is critical to delivering safe, quality patient care.”
Education: Postsecondary practical nursing program that can typically be completed in under two years. LPNs also must pass the National Council Licensure Examination-LPN (NCLEX-LPN) and be licensed in the state in which they practice.
Job description: LPNs provide basic nursing care for stable patients in settings such as nursing homes, hospitals, clinics, and in a patient’s home. They assist and support RNs and other healthcare providers and serve as an important member of a patient’s healthcare team.
Certifications: LPNs can earn certifications to strengthen their skills and help create more professional opportunities. In addition to commonly required certifications such as basic or advanced life support, three popular certifications are:
- IV Therapy Certification: This certification allows LPNs to administer IV therapies.
- Wound Care Certification (WCC): With this certification, LPNs are qualified to clean and treat common wounds. This is a popular certification for LPNs working in hospitals, skilled nursing, and long-term care.
- Certified Hemodialysis Nurse (CHN): LPNs with this certification can work in dialysis centers.
Candidates for this Job: LPNs must be ready to take on any challenge they encounter in a fast-paced healthcare environment. Successful LPNs are skilled communicators who excel in a team-based setting. If you’re ready to pursue a career in nursing but can’t commit to the 2-4 years it takes to earn a bachelor’s degree, earning an LPN certificate can be a good choice.
Salary and Job Outlook: The median annual salary for an LPN is $62,340, according to the U.S. Bureau of Labor Statistics (BLS). The BLS projects job growth for LPNs at 2.6% through 2034, the same rate for jobs overall.
Registered Nurse (RN)
Registered nurses have an Associate Degree in Nursing (ADN) or a Bachelor of Science in Nursing (BSN). The American Association of Colleges of Nursing (AACN) has recognized the BSN as the minimum education requirement, and many healthcare facilities, especially hospitals, have started to require all nurses to have a bachelor’s degree. Some also are requiring nurses on staff who have an ADN to return to school to earn a BSN.
“As an RN, we must understand a range of nursing knowledge and science to provide patient care in widely diverse healthcare settings,” says Kniewel. “But at our core, we serve as an advocate to our patients and their families with caring and compassion.”
Many healthcare facilities, especially hospitals, have started to require all nurses to have a bachelor’s degree. Some also are requiring nurses on staff who have an ADN to return to school to earn a BSN.
Education: Associate degree or bachelor’s degree. An ADN takes two years to complete and prepares nurses for general clinical tasks such as monitoring patients and performing basic bedside procedures. A bachelor’s degree takes four years to complete and offers a more advanced education that includes courses in management and leadership. ADN and BSN graduates must pass the national NCLEX-RN exam and obtain a license to practice.
Job Description: RNs manage individualized care for ill, injured, and disabled patients. This requires being able to identify a patient’s needs and collaborating with other healthcare providers to make sure patients receive appropriate treatment. RNs work in many settings, including hospitals, outpatient clinics, schools, skilled nursing facilities, inpatient rehabilitation centers, and long-term care facilities.
“The RN is the right hand of healthcare providers, providing critical information to improve patient outcomes,” says Kniewel. “We work face-to-face with both patients and their families and are often the most consistent point of contact for patients.”
Certifications: RNs may choose to pursue specialty certifications to demonstrate their advanced competence in certain areas. There are many certifications to choose from. Common ones include:
- Critical Care Registered Nurse (CCRN): This highly-regarded professional credential demonstrates a nurse’s advanced knowledge of caring for the most critically ill patients.
- Certified Emergency Nurse (CEN): Nurses with this certification have expertise in providing care in the ER.
- Certified Pediatric Nurse (CPN): Nurses who want to demonstrate clinical expertise in caring for children and youth can pursue this credential.
Candidates for this Job: Excellent nurses are highly adaptable, display empathy for others, and are committed to advocating for their patients. They have high attention to detail and strong problem-solving skills. They also have the stamina required to work long shifts when necessary.
Salary and Job Outlook: The annual median salary for RNs is $93,600, according to the BLS, and jobs are expected to grow by 4.9% through 2034. Since the BSN has become the standard for many entry-level positions, RNs with a bachelor’s degree may earn more and have more opportunities to advance into managerial roles.
RN Specialties
After RNs have a few years of experience, many have found their passion and choose to pursue a specialty. There are certifications for virtually all RN specialties, and earning one tells other healthcare providers and patients that you have deep expertise and knowledge in your field.
Here are just some of the specialties that RNs can pursue :
- Neonatal nurse: These nurses work with infants who are born prematurely or with conditions such as birth defects or cardiac anomalies. Most neonatal nurses work in neonatal intensive care units (NICUs), which usually are in larger hospitals.
- Forensic nurse: Nurses in this specialty work with victims of violence or abuse whose care intersects with the legal system. They work in hospitals, anti-violence programs, and psychiatric facilities. Forensic nurses also work in coroner’s offices and medical examiner’s offices, where they help investigate crimes.
- Pediatric nurse: Many nurses specialize in caring for children from birth to their late teens. Pediatric nurses often work in outpatient clinics, schools, and hospitals.
- Labor and delivery nurse: These nurses care for mothers during labor and delivery and provide initial care for newborns. They work alongside obstetricians and midwives in hospitals and birthing centers.
- Obstetrics (OB) nurse: OB nurses help their patients maintain healthy pregnancies. They work in obstetrics and gynecological offices, maternity units in hospitals, and birthing centers.
- Home health nurse: These nurses travel to care for patients where they live. This can include their homes, long-term care facilities, and rehabilitation facilities. Home health nurses may visit multiple patients a day.
- Psychiatric nurse: Psychiatric nurses work with individuals with behavioral or mental health challenges. They work in inpatient psychiatric units, clinics, rehabilitation centers, schools, and government agencies.
- Geriatric nurse: These nurses provide compassionate care for older patients. They work in long-term care facilities, skilled nursing units, hospitals, and clinics.
- Oncology nurse: Oncology nurses work with patients who are undergoing cancer treatment. They may work in oncology units in hospitals, outpatient treatment centers, or specialized care facilities.
- Acute care nurse: These nurses are dynamic problem-solvers who care for critically ill patients in hospitals.
- Informatics nurse: Instead of working at the bedside, informatics nurses help develop and improve healthcare communications and information technologies. They work in hospitals and outpatient treatment centers.
Candidates for this Job: Excellent nurses are highly adaptable, display empathy for others, and are committed to advocating for their patients. They have high attention to detail and strong problem-solving skills. They also have the stamina required to work long shifts when necessary.
Salary and Job Outlook: The annual median salary for RNs is $93,600, according to the BLS, and jobs are expected to grow by 4.9% through 2034. Since the BSN has become the standard for many entry-level positions, RNs with a bachelor’s degree may earn more and have more opportunities to advance into managerial roles.
Advanced Practice Registered Nurse (APRN)
Advanced practice registered nurses have either a Master of Science in Nursing (MSN) or a Doctor of Nursing Practice (DNP). These highly educated nurses have the skills to assess, diagnose, and treat patients. Depending on where they practice, many APRNs have the same authority as physicians, including managing a patient’s overall care as a primary care provider and prescribing medications.
“Holism is a hallmark of nursing and is a reason many patients and families prefer the care they receive from APRNs,” says Hilary Applequist, DNP, APRN-NP, ACHPN, a board-certified adult/gerontology nurse practitioner in Nebraska. “We look at them as whole people, not just a disease to fix. APRNs are strong patient and family advocates. We see this as a core of our vocation.”
Depending on where they practice, many APRNs have the same authority as physicians, including managing a patient’s overall care as a primary care provider and prescribing medications.
There are four types of APRNs: certified nurse midwife, certified registered nurse anesthetist, certified nurse practitioner, and clinical nurse specialist. All APRNs must be licensed in the state in which they practice. As the health industry expands, there is significant demand for APRNs.
Certified Nurse Midwife (CNM)
Education: Master of Science in a nurse-midwifery program. A master’s degree generally takes two years to complete.
Job Description: CNMs are legally recognized to practice in all states, as well as in the District of Columbia. The scope of their practice is regulated at the state level, so their roles can vary somewhat. CNMs support mothers and their partners throughout pregnancy, during labor and delivery, and postpartum. In addition, they provide gynecological and reproductive care and education.
Certification: CNMs must graduate from an accredited graduate-level midwifery program and then pass a board examination to earn their professional designation of Certified Nurse Midwife.
Candidates for this Job: Empathetic, caring nurses who want to support families throughout their pregnancy journeys make great CNMs. Emotional and mental strength is required to effectively handle the rare but heartbreaking losses that can be experienced during pregnancy.
Salary and Job Outlook: Certified nurse midwives earn a median annual salary of $128,790, according to the BLS, and the demand for these nurses is above average. The BLS says jobs for CNMs will grow by 11.1% through 2034.
Certified Registered Nurse Anesthetist (CRNA)
Education: Master of Science in Nursing in a nurse anesthetist program. This will change in 2025 when all graduating CRNAs will be required to have a DNP. A master’s generally takes two years to complete, while a doctorate takes three years.
Job description: Certified registered nurse anesthetists administer anesthesia and other medications during surgery and other medical procedures. They work in hospitals, emergency rooms, and outpatient surgical clinics, educating patients about anesthesia and identifying potential risks.
Certifications: All practicing CRNAs have passed the certification exam administered by the National Board of Certification and Recertification for Nurse Anesthetists (NBCRNA). CRNAs must be recertified every four years and retake the exam every eight years.
Candidates for this Job: RNs who have spent time in intensive care units have a solid knowledge base for pursuing a career as a CRNA. Critical-thinking skills, stamina, and attention to detail are important for this role.
Salary and Job Outlook: Certified registered nurse anesthetists generally earn significantly more than other advanced practice registered nurses. Their median annual salary is $223,210, according to the BLS, which says demand for CRNAs is high with job growth projected at 8.6% through 2034.
Nurse Practitioner (NP)
Education: Master of Science in Nursing or Doctor in Nursing Practice.
Job Description: Nurse practitioners provide primary, acute, and specialty healthcare to patients across the lifespan, within the scope of practice in their state. Increasingly, they are primary care providers for many patients.
“Nurse practitioners bring previous nursing experiences to bear as we move into the provider role, which strengthens our ability to care for individuals and families while collaborating effectively with our nurse colleagues,” says Applequist, who teaches full time in the NP program at Nebraska Methodist College.
Certifications: Nurse practitioners must pass a board examination to earn certification. They can choose from a variety of certifications, many of them for specialties. Three common certifications are:
- Family Nurse Practitioner (FNP): For nurse practitioners who care for patients across the lifespan, from birth to death.
- Adult-Gerontology NP (A-GNP): For NPs who care for adults young and old.
- Emergency NP (ENP): For nurse practitioners who practice emergency care for all ages.
Candidates for this Job: RNs who are looking to practice with autonomy. Confidence, knowledge, critical thinking, empathy, and compassion are characteristics that benefit a nurse practitioner.
Salary and Job Outlook: Nurse practitioners earn a median annual salary of $129,210, according to the BLS, and they are in high demand with projected job growth of 40.1% through 2034.
Clinical Nurse Specialist (CNS)
Education: Masters of Science in Nursing or Doctor of Nursing Practice
Job Description: Clinical nurse specialists use their advanced knowledge and skills to assess, diagnose, treat, and manage patient care. They may also work in research or management, leading nursing teams and ensuring that evidence-based practices are adopted at the team and department levels.
Certification: In most states, CNSs must earn certification in the population area in which they practice. These include:
- Adult/Gerontology
- Pediatrics
- Neonatal
Candidates for this Job: Confident, compassionate RNs who can read, interpret, and integrate scientific evidence and manage time well are strong candidates for this role.
Salary and Job Outlook: Although clinical nurse specialists are APRNs, the BLS currently classifies them as RNs, who earn an annual median salary of $93,600. RN jobs are expected to grow by 4.9% through 2034.
The BLS says that RNs like CNSs who diagnose and treat patients can earn a median salary of $100,300. However, as APRNs with graduate degrees and increased responsibilities, most CNSs likely earn salaries that fall within APRN earning ranges.







